'Hospitals not designed for pandemic'~Dr Garcia
May 13, 2020 | Expert Insights
The webinar was organized on 17th April 2020, to understand the challenges faced by frontline doctors with regards to COVID-19 pandemic and to develop a strategic vision to combat the contagion.
The panellist consisted of eight practising doctors from the United States and India namely - Dr.Jacob Anthony Kalliath, Physician in Internal Medicine, Swedish Covenant Hospital, Chicago, Illinois ,Dr.Shameeke Taylor, Emergency Medical Physician, Mount Sinai Medical Centre, New York, Dr.Richard Garcia, Medical Director – Chief of Staff, Ferry County Memorial Hospital, Washington, Dr.Matthew Anthony Kalliath, Chief Surgical Resident, University of Pennsylvania Medical Centre, Harrisburg, Dr.Jake Moore, Emergency Medical Physician, Rush Oak Park Hospital, Chicago, Dr.Anthony Kalliath, Hematologist & Oncologist, Florence – Alabama, Dr.Anoop Hajela, President United Doctors Federation, Bhopal and Dr.Gloria Alexander, BC Roy Awardee & Specialist in Infectious Diseases. The session was moderated by Major General Moni Chandi (retd), Chief Strategy Officer, Synergia Foundation
Dr Garcia emphasised the need for more testing, setting up of mobile testing facilities and contact tracing as he drew an interesting analogy, by comparing the populations of European countries to that of the states of the US. This was needed to monitor the progress of the contagion.
Another challenge faced by the front line doctors was the shortage of Personal Protective Equipment, according to Dr Jacob Kalliath, and this was a major concern. He pointed out that as the pandemic is unprecedented, doctors were learning on the job along with the progress of the pandemic. At this juncture, there are differences in professional opinion, as not enough medical literature is available. There is scope for innovation and improvisation, while the knowledge about the coronavirus improves. He also admitted that he was changing his technique of patient management, with experiencesgained.
During the discussion, the moderator brought out the current status of the Pandemic:
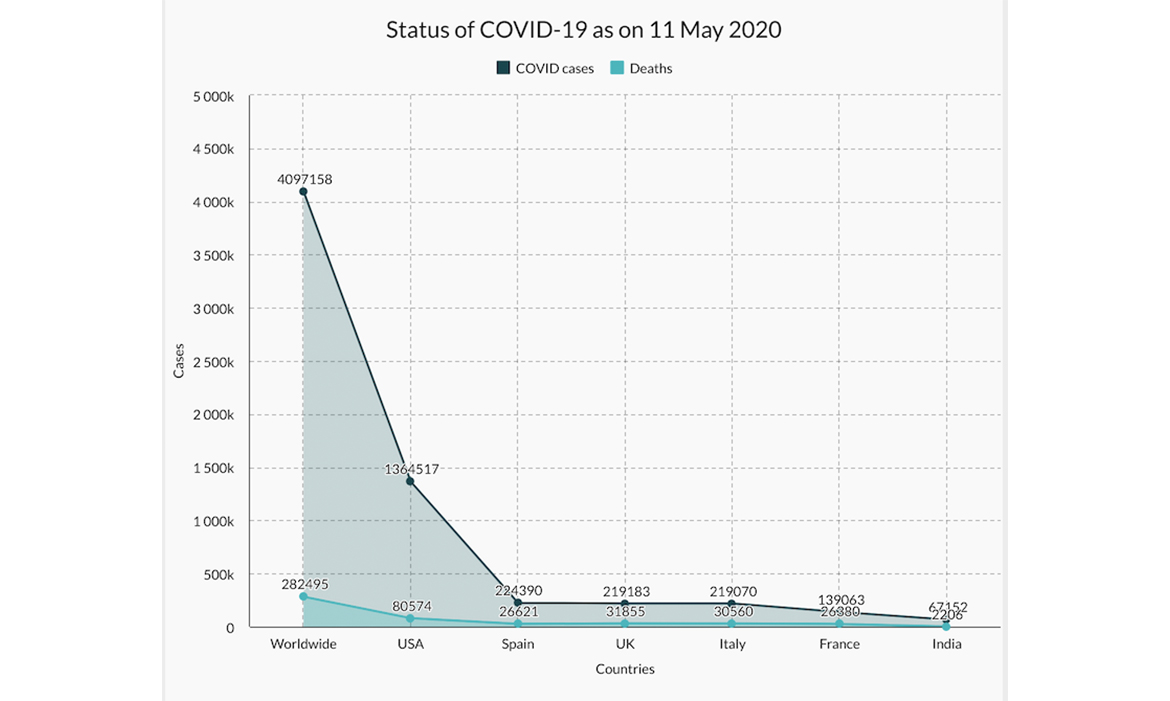
Dr Taylor gave insights on the situation in New York. He believed the peak at Mt. Sinai Hospital, NY of 800 patients a day, had been crossed a few days earlier. It was currently 600 cases a day, but authorities were wary of possible resurgence. He said 80% of the hospital load was devoted to COVID-19 patients. There were serious challenges in logistics but that innovative means were being used to fill gaps; e.g. face masks were being diverted from construction workers and 3D printers were being used for making face shields. At the time of the peaks, there is challenge for space; while available spaces will have to be reorganised, establishing robust triaging systems can reduce the load. He said that the hospital had received valuable community support, in provision of food and volunteer service. In order to reduce hospital load, some patients with breathing difficulties were sent home with oxygen cylinders and advised followed up medical checks. There are special challenges for Human Resource also - to include rotation of shifts, flexibility in scheduling, employment of volunteer staff and ensuring correct wearing of PPE by the staff.
It was also important to monitor staff for possible infection and this meant setting up kiosks in hospitals for checking fever, asking questions about travel & contacts and restraining those suspected. He also stressed the need for dynamic inventory management, to anticipate demand and more flexibility in financial controls.
As a professional surgeon, Dr Mathew Kalliath pointed out that during the pandemic, he is often confronted with the question, ‘Does the risk (of COVID infection) outweigh the benefit (of immediate surgery)?’. He also said that it was required to limit contact between people in Operating Rooms as well as deal with the concern that the coronavirus could spread aerially during the surgery. Hence the necessity to wear PPE and face shields. For the present, due to shortage of face shields, N95 masks are being used, in lieu. He said, the air filtration pump system used in laparoscopic surgery, holds promise. He also said that air-conditioning systems should be upgraded to ensure the filter is effective against the COVID-19 virus. Work-shifts in hospitals should be reorganised to cater for the longer-term of battle with the coronavirus.
Dr Jake Moore presented an interesting case that while waiting for the onslaught of the disease, the first two victims were physicians, in the hospital. Since there are no special symptoms and most people are asymptomatic, the spread of the pandemic is largely silent (invisible). He brought out the need for society to adopt new norms of social behaviour, to check the spread of the coronavirus. It was possible for people inadvertently carrying the virus from hospitals on their shoes; hence the need for disposable shoe covers and disinfecting shoes before entering one’s home. He also stressed the importance of regular and accurate messaging about the pandemic. Emphasizing the need for social messaging, he said, “Everyone appreciates knowing the hard truths about the pandemic”. People should be informed about the risks and not be kept in the dark. He said to augment the workforce during the pandemic, students from medical colleges and nursing schools could be temporarily reassigned.
Dr Anthony Kalliath explained several measures to reduce human contact, while receiving medical treatment. He emphasized the need to follow visitor protocols, patient protocols and protect staff from possible infection. He recommended tele-medicine, changing medication to make visits of existing patients to hospitals less frequent and postponing elective surgeries, to reduce patient load, during the pandemic. He said as preparation, people should strengthen innate immunity through good health practices, vitamins, supplements etc.
Dr Anoop Hajela gave an overview of arrangements made in the state of Madhya Pradesh, as preparation for the pandemic. He said major hospitals in Bhopal and Indore had been designated COVID hospitals, and smaller hospitals were designated for non-COVID treatments. He emphasized the need to protect health workers, pointing out that several employees from the Department of Health and Police had been infected because of inadequate protection (PPE). He said the government had also established several helplines, to assist people with information.
Dr Gloria Alexander gave an overview of the response made by the state of Karnataka. She said that of the approximate 80 cases in the state, 20 were treated in the private hospitals, while the remaining were treated in government hospitals. The lockdown had given time to prepare for the pandemic; hospitals now have separate COVID clinics, where patients are checked and referred to designated government hospitals, if they show symptoms of infection. The Karnataka helpline was getting more than 2000 calls per day. The helpline was being manned by students of pharmacy and MBBS. The doctor also drew an interesting comparison between the COVID and HIV viruses. India has the 3rd highest number of HIV cases, in the world. Both COVID and HIV are RNA viruses, but spread very differently. The panic over COVID is similar to that seen for HIV. She said that the medical procedure for blood plasma with antibodies was showing promise in management of COVID; however, this was not recommended for HIV.
In the question and answer sessions, some more insights were shared by the speakers. Dr Thomas said that we should pre-emptively deal with the possibility of stigmatising COVID patients. We need to deal with infection professionally and stigmatisation, like initially seen in case of HIV, would be detrimental to containing the spread of the virus. He also voiced concern about changes needed in regular hospitals, in view of the pandemic and the inaccuracy in current COVID testing procedures. He said it might be best if the ICMR laid down comprehensive protocols, on both issues.
Responding to Dr Anoop Hajela questions -- 1. Are there separate hospitals for COVID in the US? 2. Due to shortage of testing kits, does the US follow the procedure of pool testing? 3.How are hospitals in the US sealed from the COVID virus? -- were Dr Taylor and Dr Gracia. Dr Taylor said that additional bed-capacities had been set up in proximity to existing hospitals like the Kennedy Centre etc.; essentially, to decompress hospitals. Emergency services in hospitals were physically separated. Drive through testing centres have also been set up, to improve the quality of monitoring.
Finally, in Dr Gracia's opinion, it is important for people to understand that ‘Testing isn’t treatment’. Testing only helps in monitoring the spread of the infection and is a valuable input for planning counter-measures. We need to improve the quality of social messaging. Currently, hospitals have separate COVID floors for COVID patients, but this has caused cases to spill over to other (non-COVID) floors.



Comments